Breaking: CMS admits over 3.0 MILLION have already lost ACA coverage so far this year

So, what does this mean for monthly effectuated enrollment this year? Well, it's pretty safe to say that it's not going to look anything like the ePTC years [ie, 2021 - 2025]; in fact, at least a half-dozen state-based ACA exchanges have posted press releases warning that they're already seeing record levels of plan cancellations.
Instead, it seems pretty clear that the pattern is much more likely to resemble one of the NON-ePTC years. Here's what it would look like if effectuations in 2026 follow the exact path of those years...
...Depending on which year it mimics, average 2026 effectuations will range somewhere between 18.2 million - 20.9 million per month. If so, this would mean anywhere from 1.4 - 4.1 million fewer exchange enrollees than 2025.
...Of course it's also conceivable that the actual 2026 pattern won't resemble any of these; it could be higher or lower. Personally, I suspect it will be lower, with a steeper drop-off in the first quarter of the year, followed by more gradual attrition as the rest of 2026 passes by.
Paige Cunningham, NOTUS, this morning:
More than one in five people who enrolled in health insurance through HealthCare.gov during open enrollment and in the weeks immediately following were dropped from coverage for failing to pay their first month’s premium, according to internal Centers for Medicare and Medicaid Services, or CMS, documents obtained by NOTUS that haven’t been made public.
The roughly 21% decline in enrollment in the 30 states using the federal marketplace is significantly higher than the rate of last year, when 12% of enrollees dropped off over the same time frame.
...This year also saw fewer sign-ups to begin with, leaving total ACA enrollment at around 19 million people, around 3 million fewer than one year ago, according to CMS documents.
...Nationally, ACA enrollment has declined somewhat less — around 17% percent — between February and April. That’s because the 20 states running their own marketplaces were able to retain far more customers, losing 8% since the beginning of the year, according to the CMS documents.
Cunningham's story doesn't include state-level details (nor does it provide effectuated numbers for January, February or March), but there's still a lot to digest even in the top-line numbers.
NATIONALLY:
- In 2025, 24.3 million people selected policies during the Open Enrollment Period (OEP), with 22.2 million having effectuated coverage in April. That's a net drop of 8.8%.
- In 2026, 23.1 million people selected policies during OEP. If you take that 17% drop figure literally, that would put April effectuated enrollment at just 19.2 million.
That's a whopping 3.0 million fewer people with effectuated ACA exchange coverage in April 2026 vs. a year earlier.
By also providing the percent drop-off for the 30 states hosted on the federal platform (HealthCare.Gov), Cunningham also allows me to estimate the breakout between HC.gov states and the 21 states operating their own ACA platform...although this also requires adjusting each due to Illinois transitioning from the federally-facilitated marketplace (FFM) in 2025 to a state-based marketplace (SBM) in 2026:
- 2025 OEP plan selections: 17.13 million FFM, 7.19 million SBM
- 2025 April Effectuated enrollment: 15.37 million FFM, 6.82 million SBM
- 2026 OEP plan selections: 15.77 million FFM, 7.36 million SBM
- 2026 April Effectuated enrollment*: 12.46 million FFM, 6.74 million SBM
When you adjust for Illinois shifting from an FFM to a SBM state this year, it looks like this:
- 2025 OEP plan selections: 16.66 million FFM, 7.66 million SBM
- 2025 April Effectuated enrollment: 14.94 million FFM, 7.25 million SBM
- 2026 OEP plan selections: 15.77 million FFM, 7.36 million SBM
- 2026 April Effectuated enrollment*: 12.46 million FFM, 6.74 million SBM
*(assumes FFM dropped exactly 21% & the combined total dropped exactly 17% from the OEP figures)
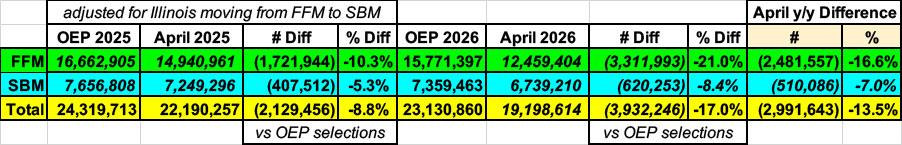
Here's what this looks like lined up side by side:
In other words, taking the 17% national & 21% FFM drops literally, that would mean nearly 2.5 million enrollees have lost coverage across the 30 states hosted by HealthCare.Gov this year (a 16.6% year over year drop), while just over 500,000 have lost coverage across the remaining 21 states which operate their own exchanges (a 7% y/y drop).
While both of these are ugly, the special programs put into place by over half of the latter states (mostly consisting of supplemental state-base subsidies & Basic Health Plan programs as well as embracing Premium Alignment) have clearly been extremely effective at helping mitigate the coverage losses. By an amazing coincidence, 16 of the 21 SBM states also happen to be controlled by Democrats, including 12 of the 13 states with either state subsidies or BHP programs in place (Oregon is the sole state w/a BHP program hosted on the federal exchange...until next year, when the state moves to its own ACA exchange).
While several FFM & GOP-controlled states do have Premium Alignment pricing policies in effect (especially Texas), most of them don't, and none of them have state-based subsidies in place...resulting in coverage losses 2.4x higher on a percentage basis and five times higher in raw numbers than the states operating their own platforms.
So, how many more enrollees will likely lose coverage over the remaining 8 months of 2026? Well, going back to my analysis from January, here's what it would look like assuming the remainder of the year follows the 2025, 2019 or 2016 models...and I'm pretty sure the 2025 model isn't in the cards at this point.
A 2016 pattern would end December with just 16.3 million enrolled in effectuated coverage for an average monthly enrollment of around 18.4 million, down nearly 4 million people vs. the 2025 monthly average.
Keep in mind however that even that would be at the low end of the range of people losing ACA exchange coverage according to a projection published by Wakely Consultants, one of the world's leading actuarial firms last month.
The other big question is which enrollees have dropped coverage so far: The lowest income brackets or those of more moderate incomes; those enrolled in high-deductible Bronze plans, low-deductible Gold or those in between, etc? Unfortunately, that type of data also likely won't be available for awhile; Cunningham's story does include a few additional data points.
Naturally, Dr. Oz, CMS & the Trump Regime are trying to pin pretty much all 3 million Americans who have lost ACA healthcare coverage so far on "fraud," although to Cunningham's credit, she's not buying that one bit:
Faced with such a stark drop in enrollment, leadership at CMS, which is led by Administrator Mehmet Oz, is seeking to attribute a majority of the enrollment declines to rooting out fraud rather than people not paying their premiums, according to three CMS sources. The sources said it’s unlikely fraud is behind most of the cancellations.
While marketplace fraud has been a problem in recent years, partly because insurance agents and brokers exploited Biden administration policies allowing year-round sign-ups, it’s more likely that a majority of the cancellations are among customers who were automatically reenrolled in their plans from last year and just never paid the premiums.
That happens every year, but this year’s rate of cancellations is significantly higher.
This is exactly what I and other healthcare policy wonks have been expecting, and it's typical of Trump Regime "logic:"
- If they kill a random Venezuelan fisherman via an airstrike, that "proves" they were a drug dealer by definition.
- If someone loses healthcare coverage due to their policies, it "proves" they were enrolled fraudulently by definition.
Anyway, I'm still not expecting the official effectuated enrollment data for the first part 2026 to come out until July, but this story makes it sound like it could come out sooner than that after all, so stay tuned...